The optimal position for chest auscultation is sitting in a chair, or on the side of the bed. A chaperone should be offered for the assessment if this is considered appropriate. Listening to a patient’s chest to establish breath and any other sounds requires a quiet area, so that health professionals can fully appreciate what they hear and interpret their clinical relevance (Sarkar et al, 2015).Ĭhest auscultation requires the chest and back to be exposed, so measures should be taken to ensure the patient’s privacy and dignity is maintained at all times. Nurses need to assess individual patients for the risk of exposure to blood and body fluids (Royal College of Nursing, 2018) and to be aware of local policies for glove use.

Non-sterile gloves are not required routinely for this procedure. Nurses are advised to have a stethoscope for their own use, as sharing equipment may increase infection risk and maintaining clean ear tips can be difficult.

Adherence to local infection prevention and control policies, including the cleaning of equipment between every patient contact, is essential. The stethoscope is an important tool for clinical assessment, but can become contaminated by micro-organisms (Longtin et al, 2014). Fig 3 illustrates parts of the stethoscope. The bell of the stethoscope is generally used to detect high-pitched sounds – at the apex of the lungs above the clavicle its diaphragm is used to detect low-pitched sounds in the rest of the chest (Dougherty and Lister, 2015).
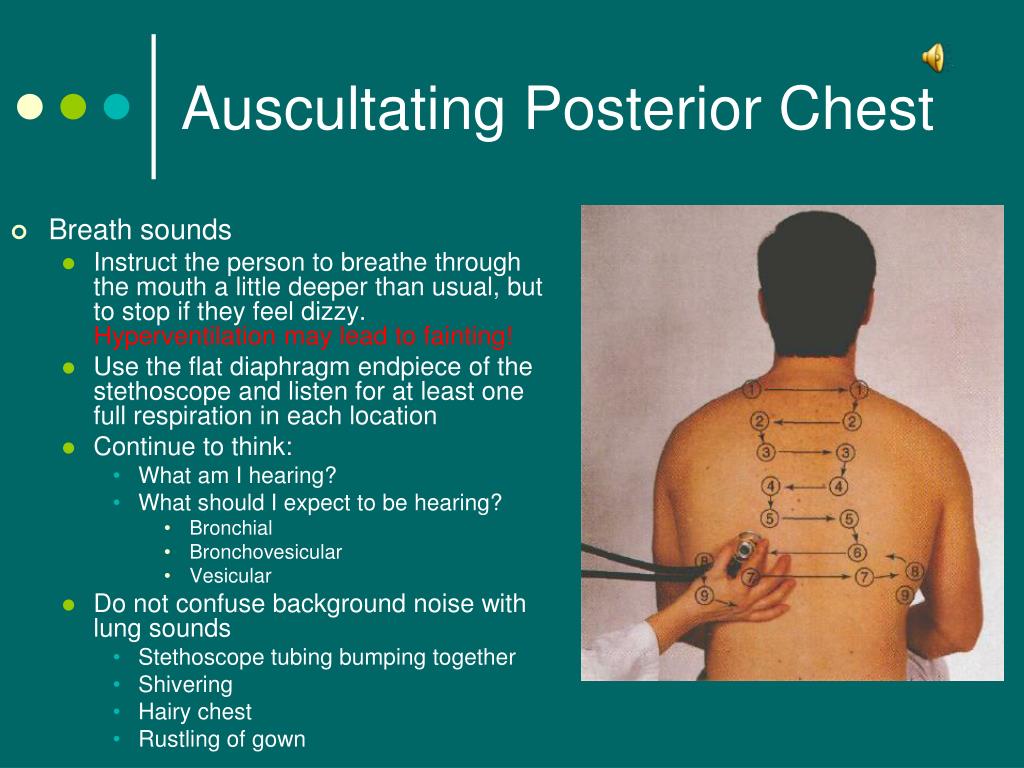
To undertake a thorough assessment of the chest, including auscultation, it is essential to understand the anatomy and physiology of the respiratory system. The Nursing and Midwifery Council (2018) has included chest auscultation and interpretation of findings in the Standards of Proficiency for Registered Nurses, and student nurses now learn this skill as undergraduates. This is an example of a systemic assessment tool but other tools are available (Simpson, 2015) The procedure should always form part of an holistic assessment and must be viewed alongside the patient’s clinical history (Box 1).Ī commonly used acronym in clinical examination of the chest is IPPA: Scroll down to read the article or download a print-friendly PDF here (if the PDF fails to fully download please try again using a different browser)Īlthough the first stethoscope for auscultation was invented in 1816 by René-Théophile-Hyacinthe Laennec, the use of auscultation dates back to Hippocrates, who would place his ear to his patient’s chest and listen for sounds.Īuscultation is an important part of an assessment of the respiratory system and is also used for cardiac and gastrointestinal examination.This article has been double-blind peer reviewed.Nursing Times 116: 1, 23-26.Īuthors: Jaclyn Proctor is respiratory advanced nurse practitioner at Warrington and Halton NHS Foundation Trust Emma Rickards is respiratory nurse consultant at Liverpool Heart and Chest Hospital NHS Foundation Trust and Knowsley Community Respiratory Service. This article explains the clinical procedure for chest auscultation and provides a guide to interpreting findings.Ĭitation: Proctor J, Rickards E (2020) How to perform chest auscultation and interpret the findings. Chest auscultation is frequently used in the clinical examination of patients.
